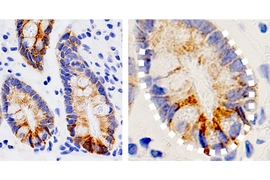
Every three to five days, all of the cells lining the human intestine are replaced. That constant replenishment of cells helps the intestinal lining withstand the damage caused by food passing through the digestive tract.
This rapid turnover of cells relies on intestinal stem cells, which give rise to all of the other types of cells found in the intestine. Recent research has shown that those stem cells are heavily influenced by diet, which can help keep them healthy or stimulate them to become cancerous.
“Low-calorie diets such as fasting and caloric restriction can have antiaging effects and antitumor effects, and we want to understand why that is. On the other hand, diets that lead to obesity can promote diseases of aging, such as cancer,” says Omer Yilmaz, associate professor of biology at MIT.
For the past decade, Yilmaz has been studying how different diets and environmental conditions affect intestinal stem cells, and how those factors can increase the risk of cancer and other diseases. This work could help researchers develop new ways to improve gastrointestinal health, either through dietary interventions or drugs that mimic the beneficial effects of certain diets, he says.
“Our findings have raised the possibility that fasting interventions, or small molecules that mimic the effects of fasting, might have a role in improving intestinal regeneration,” says Yilmaz, who is also a member of MIT’s Koch Institute for Integrative Cancer Research.
A clinical approach
Yilmaz’s interest in disease and medicine arose at an early age. His father practiced internal medicine, and Yilmaz spent a great deal of time at his father’s office after school, or tagging along at the hospital where his father saw patients.
“I was very interested in medicines and how medicines were used to treat diseases,” Yilmaz recalls. “He’d ask me questions, and many times I wouldn’t know the answer, but he would encourage me to figure out the answers to his questions. That really stimulated my interest in biology and in wanting to become a doctor.”
Knowing that he wanted to go into medicine, Yilmaz applied and was accepted to an eight-year, combined bachelor’s and MD program at the University of Michigan. As an undergraduate, this gave him the freedom to explore areas of interest without worrying about applying to medical school. While majoring in biochemistry and physics, he did undergraduate research in the field of protein folding.
During his first year of medical school, Yilmaz realized that he missed doing research, so he decided to apply to the MD/PhD program at the University of Michigan. For his PhD research, he studied blood-forming stem cells and identified new markers that allowed such cells to be more easily isolated from the bone marrow.
“This was important because there’s a lot of interest in understanding what makes a stem cell a stem cell, and how much of it is an internal program versus signals from the microenvironment,” Yilmaz says.
After finishing his PhD and MD, he thought about going straight into research and skipping a medical residency, but ended up doing a residency in pathology at Massachusetts General Hospital. During that time, he decided to switch his research focus from blood-forming stem cells to stem cells found in the gastrointestinal tract.
“The GI tract seemed very interesting because in contrast to the bone marrow, we knew very little about the identity of GI stem cells,” Yilmaz says. “I knew that once GI stem cells were identified, there’d be a lot of interesting questions about how they respond to diet and how they respond to other environmental stimuli.”
Dietary questions
To delve into those questions, Yilmaz did postdoctoral research at the Whitehead Institute, where he began investigating the connections between stem cells, metabolism, diet, and cancer.
Because intestinal stem cells are so long-lived, they are more likely to accumulate genetic mutations that make them susceptible to becoming cancerous. At the Whitehead Institute, Yilmaz began studying how different diets might influence this vulnerability to cancer, a topic that he carried into his lab at MIT when he joined the faculty in 2014.
One question his lab has been exploring is why low-calorie diets often have protective effects, including a boost in longevity — a phenomenon that has been seen in many studies in animals and humans.
In a 2018 study, his lab found that a 24-hour fast dramatically improves stem cells’ ability to regenerate. This effect was seen in both young and aged mice, suggesting that even in old age, fasting or drugs that mimic the effects of fasting could have a beneficial effect.
On the flip side, Yilmaz is also interested in why a high-fat diet appears to promote the development of cancer, especially colorectal cancer. In a 2016 study, he found that when mice consume a high-fat diet, it triggers a significant increase in the number of intestinal stem cells. Also, some non-stem-cell populations begin to resemble stem cells in their behavior. “The upshot of these changes is that both stem cells and non-stem-cells can give rise to tumors in a high-fat diet state,” Yilmaz says.
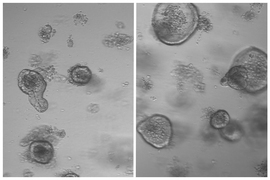
To help with these studies, Yilmaz’s lab has developed a way to use mouse or human intestinal stem cells to generate miniature intestines or colons in cell culture. These “organoids” can then be exposed to different nutrients in a very controlled setting, allowing researchers to analyze how different diets affect the system.
Recently, his lab adapted the system to allow them to expand their studies to include the role of immune cells, fibroblasts, and other supportive cells found in the microenvironment of stem cells. “It would be remiss of us to focus on just one cell type,” Yilmaz says. “We’re looking at how these different dietary interventions impact the entire stem cell neighborhood.”
While Yilmaz spends most of his time running his lab at MIT, he also devotes six to eight weeks per year to his work at MGH, where he is an associate pathologist focusing on gastrointestinal pathology.
“I enjoy my clinical work, and it always reminds me about the importance of the research we do,” he says. “Seeing colon cancer and other GI cancers under the microscope, and seeing their complexity, reminds me of the importance of our mission to figure out how we can prevent these cancers from forming.”