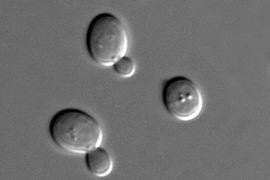
Yeast populations exposed to a sudden environmental shock can be driven to extinction, MIT researchers have shown. Could this principle also apply to human cancer cells? Possibly, argue researchers from MIT, Boston University, and Memorial Sloan-Kettering Cancer Center in a Perspectives article published online on April 17 by Nature Reviews Cancer and appearing in the May 2014 print edition.
Tools from ecology and evolution are bringing about new ways to think about cancer and new pathways for fighting its development and spread. These tools include population dynamics, evolutionary game theory, frequency dependent selection and critical slowing down, genetic drift, and spatial diversity.
In the article, co-authors Kirill Korolev, assistant professor of physics at Boston University, Joao B. Xavier, computational biologist at Memorial Sloan-Kettering Cancer Center, in New York, and Jeff Gore, Latham Family Career Development Assistant Professor of Physics at MIT, suggest that evidence from natural population extinctions and from theoretical and empirical studies points to new ways of guiding drug delivery by identifying the threshold population size for cancer cells to form a tumor.
"By thinking about cancer cells as an endangered species, cancer vulnerabilities become more apparent," the authors say in their abstract.
Just as fish swim in schools to avoid predators, it may be that cancer cells cooperate and that they must reach a certain threshold population before they can form a tumor. A number below that threshold may lead to extinction of those cells.
Researchers at Princeton, University of California-San Francisco, and the Salk Institute argued similarly in a May 2011 Perspectives article in Nature Reviews Cancer that bacterial populations, which have much in common with human cancer tumors, could serve as a biological model for scientific studies of adaptation and evolution.
The new Perspectives piece grew out of work at the Gore Laboratory at MIT, where lead author Korolev previously served as a Pappalardo Postdoctoral Fellow. In nature, an organism may thrive at an intermediate population size but fail when that population grows too small. This phenomenon, called a strong Allee effect, has been observed in laboratory cell cultures, where it is hard for an individual cancer cell to grow by itself in isolation unless the media is conditioned by secretions from other cells, the authors note. Similarly, small groups of cancer cells that spread from their original site may stay dormant for a long time. Allee effects might open several new mechanisms for cancer treatment, such as drugs that reduce the number of cells below the threshold for survival or raise the threshold for tumor formation by interfering with cooperative growth among cancer cells. "A radically new approach to therapy would be to focus on the size of the threshold, rather than on the population size," the authors suggest.
The fact that some cancers return after treatment seems to contradict this argument, or at least point to an alternative route for tumor formation. Since cancer is typically a collection of a variety of mutated cells rather than a single deformed line, recurrence could indicate either that some cells remained after treatment that had weak or absent Allee effects or that some left-over cancer cells continued to mutate during remission, becoming more potent tumor formers.
One hope from the new approach is that identifying and targeting Allee effects could block the spread of cancer from the primary site. "Even a modest increase in the size of the growth threshold can yield a marked reduction in the probability of successful metastasis being formed," the authors wrote. For existing tumors, traditional cancer treatments would still be needed at the primary site, but that treatment "would push the primary tumor below the critical population size and lead to a rapid population 'meltdown.' Here, again, high growth thresholds could be beneficial, because they make it harder for new mutations to rescue the population."
Complex interactions between prostate cancer cells, for example, and the body's macrophages (white blood cells) and stromal cells (connective tissue) can change the body's natural environment, creating a new ecology that favors tumor formation. Targeting not only the cancer cells but also the altered blood cells or tissue cells could create a new route to stop the spread of the cancer. The drug clodronate, for example, is used to block the spread of breast cancer to the bone. "As mutations tend to vary across patients, whereas stromal cells do not, therapies that target the stroma may have wider applicability than therapies that target somatic mutations," the authors wrote. (Somatic mutations are ones that are not inherited.) Other researchers have applied evolutionary game theory models to explore cancer spread in multiple myeloma, a cancer affecting specialized white blood cells called plasma.
Because of their genetic diversity, several variant cancer cell lines, each adapted to carry out different functions, could exist simultaneously as a small proportion of the overall tumor population. For example, some cancer cells could carry lower rates of natural cell death (apoptosis), while others add the ability to recruit blood vessels. Such interdependency of related but differently adapted cells raises the possibility of additional strategies to fight the cancer, such as attacking the weakest cell line needed to support the tumor or increasing the interdependencies of different cell lines, making it harder for them to spread and form remote tumors.
Previous research by Gore and Alvaro Sanchez, a former MIT postdoctoral associate who is now a junior fellow at the Rowland Institute of Science at Harvard University, demonstrated that a mixed population of “cooperators” and “cheaters” in yeast responded to stress by altering the mix of cooperators and cheaters. Given sufficient time, the population evolved to reach a new stable state, but a sudden stress caused the population to collapse. If cancer cells behave in a similar way, this suggests that time is the enemy in terms of controlling cancer, and that a sudden shock will have the best results against it. Thus, cancer should be "hit hard," the new article proposes.
Robert Austin, professor of physics at Princeton University, says of the Nature Cancer Reviews piece, “I think this perspective is interesting, but maybe needs to look more carefully at some of the experiments that already exist that would indicate that things are not as simple or optimistic as you might hope.” In a truly complex ecology, Austin says, there is always a place for a mutant to slowly grow and increase fitness. In a September 2011 Science paper, with lead author Qiucen Zhang, Austin and colleagues developed a complex ecology to accelerate the evolution of drug resistance in bacteria. “The problem is, that experiment showed that even with only 100 bacteria in the initial inoculation, the eventual emergence of drug resistance was inevitable,” he says.
Korolev also previously studied the role of tumor cells known as "passenger" cells in the MIT lab of Leonid Mirny, associate professor of health sciences and technology and physics in the Harvard-MIT Division of Health Sciences and Technology. As a mutation-driven asexual evolutionary process, cancer may follow the same evolutionary dynamics as viruses and bacteria. One possible consequence of such a process is that small tumors produce mutations that are less able to reproduce themselves and shrink, while large tumors produce more self-sustaining mutations, called drivers, and grow. "The critical population size, which controls the ability of the tumor to adapt, depends on evolutionary parameters of the cancer," Gore and colleagues argue. That opens pathways to interfere with the evolutionary dynamics of the cancer. "Mutation rates can be increased by adding a mutagen or by inhibiting DNA repair machinery."
Animal tests to measure threshold size may be possible by targeting a tumor with pulsed application of a drug and studying the response. If tests show that a large attack shrinks the tumor and leads to remission while a smaller attack at first shrinks the tumor but then lets it rebound, that split response would indicate a potential Allee threshold and prescribe a minimum level for effective drug dosage.
"When replica experiments are possible, a direct way to ascertain a growth threshold is to measure how the probability of remission depends on the initial size of the tumor," they say. "Given the complexity of cancer, it would be remarkable if such simple techniques can succeed at identifying thresholds in cancer dynamics. Nevertheless, their success in natural populations suggests that some potentially cancer-specific indicators of thresholds can be identified and deployed in laboratory-based research and in the clinic."
Like expansions of wild animal populations, tumor growth shows spatial diversity, with similar mutations clustering to the exclusion of other variants. The segregation is helped along by genetic drift, which is random fluctuations in the number of successive generations from a cancer cell line, and it might be limited by nutrient control. Studies by other researchers have shown that such genetic variety in tumors can produce faster cancer cell evolution and lead to more aggressive cells. These findings suggest that inclusion of evolutionary and ecological factors in cancer drug development is an important next step, Gore and colleagues offer in their opinion piece.
"The authors did a great job in summarizing a difficult topic and weaving together many different threads of research," says Dr. Robert A. Gatenby, chair of radiology at the Moffitt Cancer Center in Tampa, Fla. "It is likely that evolution represents the first principles of cancer, but it is important to recognize that cancer also has an ecology that causes spatial and temporal heterogeneity, which strongly affects therapeutic outcome. While the conceptual model of cancer as evolution is at least 50 years old, the full implications of this paradigm in cancer treatment and prevention are only now being realized. The biggest challenge now is moving from theory to practice and using evolutionary principles in cancer therapy."
Korolev, Xavier, and Gore suggest two techniques to address evolutionary dynamics and cancer cell line evolution in tumors: lineage tracing, which has been used to identify cancer stem cells, and methylation patterns of non-expressed genes. "It remains to be seen if lineage tracing, spatially resolved sequencing or other experimental techniques can fully characterize evolutionary and ecological dynamics within the tumor, thereby opening up possibilities for accurate modeling of tumor evolution and new treatment strategies," they say.
Gore's work is supported by an NIH New Innovator Award and an NSF CAREER Award. Gore is also a Pew Scholar, Allen Distinguished Investigator, and Sloan Research Fellow. Xavier's work is supported by grants from the National Cancer Institute and the National Institutes of Health.