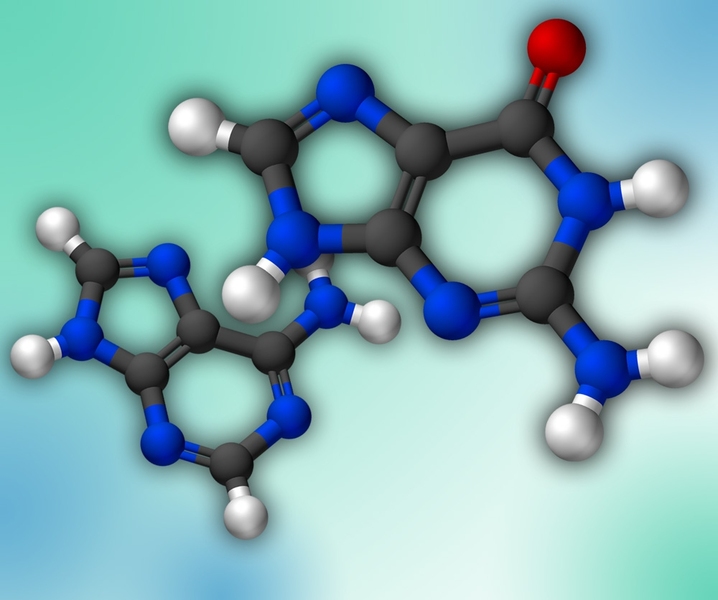
Many critical cell functions depend on a class of molecules called purines, which form half of the building blocks of DNA and RNA, and are a major component of the chemicals that store a cell’s energy. Cells keep tight control over their purine supply, and any disruption of that pool can have serious consequences.
In a new study, MIT biological engineers have precisely measured the effects of errors in systems for purine production and breakdown. They found that defects in enzymes that control these processes can severely alter a cell’s DNA sequences, which may explain why people who carry certain genetic variants of purine metabolic enzymes have a higher risk for some types of cancer.
DNA usually consists of a sequence of four building blocks, or nucleotides: adenine, guanine, cytosine and thymine (the A, G, C and T “letters” that make up the genetic code). Guanine and adenine are purines, and each has a close structural relative that can take its place in DNA or RNA. When these nucleotides, known as xanthine and hypoxanthine, are mistakenly inserted into DNA, they cause mutations. They can also interfere with the function of messenger RNA (mRNA), which carries DNA’s instructions to the rest of the cell, and the RNA molecules that translate mRNA into proteins.
“A cell needs to control the concentrations very carefully so that it has just the right amount of building blocks when it’s synthesizing DNA. If the cell has an imbalance in the concentrations of those nucleotides, it’s going to make a mistake,” says Peter Dedon, a professor of biological engineering at MIT and senior author of the study, which is appearing in the Proceedings of the National Academy of Sciences the week of Jan. 30.
In addition to forming the backbone of DNA and RNA, purines are also a major component of ATP, the cell’s energy currency; other molecules that manage a cell’s energy flow; and small chemical cofactors required for the activity of thousands of cell enzymes.
Abnormal metabolism
Dozens of enzymes are involved in purine metabolism, and it has long been known that malfunction of those enzymes can have adverse effects. For example, losing a purine salvage enzyme, which recovers purine nucleotides from degraded DNA and RNA, leads to high blood levels of uric acid, causing gout and kidney stones — and in extreme cases, a neurological disorder called Lesch-Nyhan syndrome. Losing another salvage enzyme produces a disease called severe combined immunodeficiency.
Abnormal purine metabolism can also lead to side effects for people taking a class of drugs called thiopurines. In some people, these drugs, often used to treat leukemia, lymphoma, Crohn’s disease, rheumatoid arthritis and organ-transplant rejection, can be metabolized into toxic compounds. Genetic testing can reveal which patients should avoid thiopurine drugs.
In the new study, Dedon and his colleagues disrupted about half a dozen purine metabolism enzymes in E. coli and yeast. After altering the enzymes, the researchers measured how much xanthine and hypoxanthine was integrated into the cells’ DNA and RNA, using a highly sensitive mass spectrometry technique they had previously developed to study DNA and RNA damage caused by inflammation.
They found that the malfunctioning enzymes could produce dramatic increases — up to 1,000-fold — in the amounts of hypoxanthine incorporated into DNA and RNA in place of adenine. However, they saw very little change in the amount of xanthine inserted in place of guanine.
Chris Mathews, a professor emeritus of biochemistry and biophysics at Oregon State University, says the finding could help researchers better understand how defects in purine metabolism produce disease. “This paper opens the door to numerous studies — for example, looking into the biological effects resulting from the accumulation of abnormal bases in DNA and RNA,” says Mathews, who was not involved in this study.
Scientists have found quite a bit of genetic variation in purine metabolic enzymes in humans, so the research team plans to investigate the impact of those human variants on xanthine and hypoxanthine insertion into DNA. They are also interested in studying the metabolism of the other two nucleotides found in DNA, cytosine and thymine, which are pyrimidines.
In a new study, MIT biological engineers have precisely measured the effects of errors in systems for purine production and breakdown. They found that defects in enzymes that control these processes can severely alter a cell’s DNA sequences, which may explain why people who carry certain genetic variants of purine metabolic enzymes have a higher risk for some types of cancer.
DNA usually consists of a sequence of four building blocks, or nucleotides: adenine, guanine, cytosine and thymine (the A, G, C and T “letters” that make up the genetic code). Guanine and adenine are purines, and each has a close structural relative that can take its place in DNA or RNA. When these nucleotides, known as xanthine and hypoxanthine, are mistakenly inserted into DNA, they cause mutations. They can also interfere with the function of messenger RNA (mRNA), which carries DNA’s instructions to the rest of the cell, and the RNA molecules that translate mRNA into proteins.
“A cell needs to control the concentrations very carefully so that it has just the right amount of building blocks when it’s synthesizing DNA. If the cell has an imbalance in the concentrations of those nucleotides, it’s going to make a mistake,” says Peter Dedon, a professor of biological engineering at MIT and senior author of the study, which is appearing in the Proceedings of the National Academy of Sciences the week of Jan. 30.
In addition to forming the backbone of DNA and RNA, purines are also a major component of ATP, the cell’s energy currency; other molecules that manage a cell’s energy flow; and small chemical cofactors required for the activity of thousands of cell enzymes.
Abnormal metabolism
Dozens of enzymes are involved in purine metabolism, and it has long been known that malfunction of those enzymes can have adverse effects. For example, losing a purine salvage enzyme, which recovers purine nucleotides from degraded DNA and RNA, leads to high blood levels of uric acid, causing gout and kidney stones — and in extreme cases, a neurological disorder called Lesch-Nyhan syndrome. Losing another salvage enzyme produces a disease called severe combined immunodeficiency.
Abnormal purine metabolism can also lead to side effects for people taking a class of drugs called thiopurines. In some people, these drugs, often used to treat leukemia, lymphoma, Crohn’s disease, rheumatoid arthritis and organ-transplant rejection, can be metabolized into toxic compounds. Genetic testing can reveal which patients should avoid thiopurine drugs.
In the new study, Dedon and his colleagues disrupted about half a dozen purine metabolism enzymes in E. coli and yeast. After altering the enzymes, the researchers measured how much xanthine and hypoxanthine was integrated into the cells’ DNA and RNA, using a highly sensitive mass spectrometry technique they had previously developed to study DNA and RNA damage caused by inflammation.
They found that the malfunctioning enzymes could produce dramatic increases — up to 1,000-fold — in the amounts of hypoxanthine incorporated into DNA and RNA in place of adenine. However, they saw very little change in the amount of xanthine inserted in place of guanine.
Chris Mathews, a professor emeritus of biochemistry and biophysics at Oregon State University, says the finding could help researchers better understand how defects in purine metabolism produce disease. “This paper opens the door to numerous studies — for example, looking into the biological effects resulting from the accumulation of abnormal bases in DNA and RNA,” says Mathews, who was not involved in this study.
Scientists have found quite a bit of genetic variation in purine metabolic enzymes in humans, so the research team plans to investigate the impact of those human variants on xanthine and hypoxanthine insertion into DNA. They are also interested in studying the metabolism of the other two nucleotides found in DNA, cytosine and thymine, which are pyrimidines.