There are more than 1 million blind people in the U.S., and about 100,000 of those lost their sight due to retinitis pigmentosa, a disease that destroys light-sensitive cells in the retina.
There is currently no cure for retinitis pigmentosa, but scientists are working on ways to restore vision by making other cells of the retina, which are spared by the disease, sensitive to light. In a new study of mice, researchers at the University of Southern California (USC) used technology developed by a consortium of institutions, including MIT, to do just that. By inducing light sensitivity in other cells of the retina, they brought back enough vision for the mice to navigate a maze.
Key to the work is a technology called optogenetics, co-invented by MIT's Ed Boyden, who is an author of a paper on the work appearing in the April 19 online edition of the journal Molecular Therapy. Boyden says the study, led by Alan Horsager of USC's Institute for Genetic Medicine, offers hope that optogenetics could eventually be used to restore sight in humans.
“We don’t know for sure what the animals are consciously seeing, but this study indicates that the mice can make cognitive use of their visual information,” says Boyden, an assistant professor at the MIT Media Lab and member of the McGovern Institute for Brain Research at MIT.
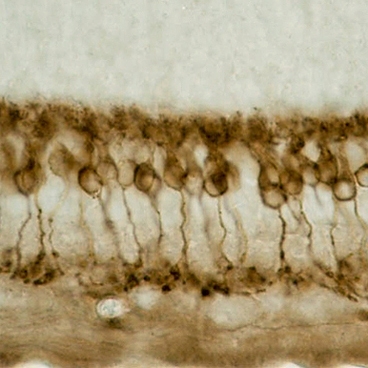
Retinitis pigmentosa can be caused by any one of more than 100 different genetic mutations, each of which leads to the gradual destruction of light-sensitive cells called photoreceptors. Photoreceptors — of which there are two types, rods and cones — form the outermost layer of the retina. They convert light into electrical signals, which are sent to neurons in the retina’s middle layer known as bipolar cells. Bipolar cells send visual information to the inner layer, made up of ganglion cells, which then connect to the brain via the optic nerve.
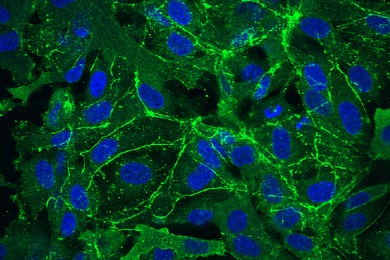
Optogenetics offers the ability to bypass damaged photoreceptors. The technology involves genetically engineering other types of cells to respond to light by adding genes that code for proteins called channelrhodopsins, which normally sit in the photoreceptor cell membrane. Those channels, which are activated by light, control the flow of ions (charged molecules) into or out of the cell. When light strikes the cell, the channels can open or close, either stimulating or suppressing the flow of ions and thus the electrical activity of the cell.
“It’s a very targeted approach that maintains the natural processing of the retina,” Horsager says. “There is a lot more to understand, but initial indications suggest we have developed something that can have enormous benefit to people. Preclinical studies are the next step to determine the potential therapeutic benefit for humans.”
Restoring light sensitivity
Over the past five years, many research groups have been exploring the possibility of restoring vision with optogenetics. In the new study, Horsager and Boyden focused on making retinal bipolar cells sensitive to light. To deliver the channelrhodopsin genes efficiently to those cells, Horsager enlisted the help of William Hauswirth, professor of genetics at the University of Florida and an expert in developing viruses that can deliver genes to the eye.
The researchers decided to target a subset of bipolar cells called ON cells. ON cells are activated in bright light, while OFF bipolar cells are suppressed in bright light. To ensure that the channelrhodopsin gene was expressed only in the ON cells, the researchers included a DNA sequence that is known to drive gene expression specifically in those cells.
The blind mice in the study had one of three different genetic mutations, all of which lead to loss of photoreceptor cells by the time the mice reach adulthood. At the age of eight weeks, the blind mice were given a subretinal injection of the virus carrying the channelrhodopsin gene. The gene was selectively integrated into the ON bipolar cells.
To test their vision, the mice were placed in a water maze with six arms branching off from a central pool. Only one arm offers an exit, which is lit up. Sighted mice quickly learn how to navigate the maze, but (untreated) blind mice have a harder time. However, they eventually learn to find their way out of the maze by trying each of the arms in turn.
At first, the blind mice treated with the channelrhodopsin gene performed similarly to the untreated mice, but after two weeks, they were able to navigate the maze just as well as the sighted mice, and much better than the untreated blind mice.
The researchers found that the effect lasted up to 10 months, the length of the study. They also found that the treatment did not provoke an immune response in the mice or any other adverse effects commonly evaluated for a new clinical technology.
Sheila Nirenberg, associate professor of physiology at Weill Medical College of Cornell University, says the study convincingly shows that the mice had some vision restored. “It’s a hard thing to do,” she says. “They successfully expressed the virus in the right cells, they got the expression to last a long time, and they showed there were no deleterious effects — all good news."
Visual input
In future work, the researchers plan to develop new behavioral tests that will help them determine what kind of visual input the mice are actually getting. For example, they could use a variation of the water maze in which the mice have to distinguish different shapes — instead of just light and dark — to learn the way out, Boyden says.
Light-sensitive proteins that can be used in optogenetics are found in a wide range of organisms, including plants, fungus and bacteria. Boyden is now screening the genomes of plants and other species to look for new channelrhodopsin-like proteins that may perform even better than the ones they are currently using.
Another important step is designing optical hardware that might be useful if this treatment is developed for human patients. For example, it might be necessary to develop goggles that transform the various light levels that a human patient might encounter in everyday life into the levels optimal for activating the light-gated channels.
There is currently no cure for retinitis pigmentosa, but scientists are working on ways to restore vision by making other cells of the retina, which are spared by the disease, sensitive to light. In a new study of mice, researchers at the University of Southern California (USC) used technology developed by a consortium of institutions, including MIT, to do just that. By inducing light sensitivity in other cells of the retina, they brought back enough vision for the mice to navigate a maze.
Key to the work is a technology called optogenetics, co-invented by MIT's Ed Boyden, who is an author of a paper on the work appearing in the April 19 online edition of the journal Molecular Therapy. Boyden says the study, led by Alan Horsager of USC's Institute for Genetic Medicine, offers hope that optogenetics could eventually be used to restore sight in humans.
“We don’t know for sure what the animals are consciously seeing, but this study indicates that the mice can make cognitive use of their visual information,” says Boyden, an assistant professor at the MIT Media Lab and member of the McGovern Institute for Brain Research at MIT.
Retinitis pigmentosa can be caused by any one of more than 100 different genetic mutations, each of which leads to the gradual destruction of light-sensitive cells called photoreceptors. Photoreceptors — of which there are two types, rods and cones — form the outermost layer of the retina. They convert light into electrical signals, which are sent to neurons in the retina’s middle layer known as bipolar cells. Bipolar cells send visual information to the inner layer, made up of ganglion cells, which then connect to the brain via the optic nerve.
Optogenetics offers the ability to bypass damaged photoreceptors. The technology involves genetically engineering other types of cells to respond to light by adding genes that code for proteins called channelrhodopsins, which normally sit in the photoreceptor cell membrane. Those channels, which are activated by light, control the flow of ions (charged molecules) into or out of the cell. When light strikes the cell, the channels can open or close, either stimulating or suppressing the flow of ions and thus the electrical activity of the cell.
“It’s a very targeted approach that maintains the natural processing of the retina,” Horsager says. “There is a lot more to understand, but initial indications suggest we have developed something that can have enormous benefit to people. Preclinical studies are the next step to determine the potential therapeutic benefit for humans.”
Restoring light sensitivity
Over the past five years, many research groups have been exploring the possibility of restoring vision with optogenetics. In the new study, Horsager and Boyden focused on making retinal bipolar cells sensitive to light. To deliver the channelrhodopsin genes efficiently to those cells, Horsager enlisted the help of William Hauswirth, professor of genetics at the University of Florida and an expert in developing viruses that can deliver genes to the eye.
The researchers decided to target a subset of bipolar cells called ON cells. ON cells are activated in bright light, while OFF bipolar cells are suppressed in bright light. To ensure that the channelrhodopsin gene was expressed only in the ON cells, the researchers included a DNA sequence that is known to drive gene expression specifically in those cells.
The blind mice in the study had one of three different genetic mutations, all of which lead to loss of photoreceptor cells by the time the mice reach adulthood. At the age of eight weeks, the blind mice were given a subretinal injection of the virus carrying the channelrhodopsin gene. The gene was selectively integrated into the ON bipolar cells.
To test their vision, the mice were placed in a water maze with six arms branching off from a central pool. Only one arm offers an exit, which is lit up. Sighted mice quickly learn how to navigate the maze, but (untreated) blind mice have a harder time. However, they eventually learn to find their way out of the maze by trying each of the arms in turn.
At first, the blind mice treated with the channelrhodopsin gene performed similarly to the untreated mice, but after two weeks, they were able to navigate the maze just as well as the sighted mice, and much better than the untreated blind mice.
The researchers found that the effect lasted up to 10 months, the length of the study. They also found that the treatment did not provoke an immune response in the mice or any other adverse effects commonly evaluated for a new clinical technology.
Sheila Nirenberg, associate professor of physiology at Weill Medical College of Cornell University, says the study convincingly shows that the mice had some vision restored. “It’s a hard thing to do,” she says. “They successfully expressed the virus in the right cells, they got the expression to last a long time, and they showed there were no deleterious effects — all good news."
Visual input
In future work, the researchers plan to develop new behavioral tests that will help them determine what kind of visual input the mice are actually getting. For example, they could use a variation of the water maze in which the mice have to distinguish different shapes — instead of just light and dark — to learn the way out, Boyden says.
Light-sensitive proteins that can be used in optogenetics are found in a wide range of organisms, including plants, fungus and bacteria. Boyden is now screening the genomes of plants and other species to look for new channelrhodopsin-like proteins that may perform even better than the ones they are currently using.
Another important step is designing optical hardware that might be useful if this treatment is developed for human patients. For example, it might be necessary to develop goggles that transform the various light levels that a human patient might encounter in everyday life into the levels optimal for activating the light-gated channels.