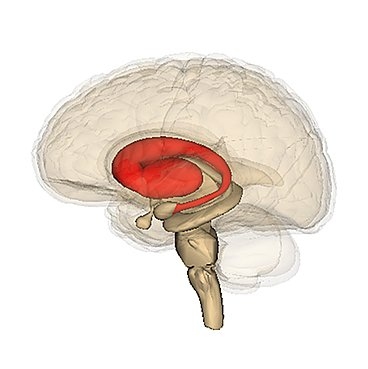
The key hallmark of Parkinson’s disease is a slowdown of movement caused by a cutoff in the supply of dopamine to the brain region responsible for coordinating movement. While scientists have understood this general process for many years, the exact details of how this happens are still murky.
“We know the neurotransmitter, we know roughly the pathways in the brain that are being affected, but when you come right down to it and ask what exactly is the sequence of events that occurs in the brain, that gets a little tougher,” says Ann Graybiel, an MIT Institute Professor and member of MIT’s McGovern Institute for Brain Research.
A new study from Graybiel’s lab offers insight into some of the precise impairments caused by the loss of dopamine in brain cells affected by Parkinson’s disease. The findings, which appear in the March 12 online edition of the Journal of Neuroscience, could help researchers not only better understand the disease, but also develop more targeted treatments.
Lead author of the paper is Ledia Hernandez, a former MIT postdoc. Other authors are McGovern Institute research scientists Yasuo Kubota and Dan Hu, former MIT graduate student Mark Howe and graduate student Nuné Lemaire.
Cutting off dopamine
The neurons responsible for coordinating movement are located in a part of the brain called the striatum, which receives information from two major sources — the neocortex and a tiny region known as the substantia nigra. The cortex relays sensory information as well as plans for future action, while the substantia nigra sends dopamine that helps to coordinate all of the cortical input.
“This dopamine somehow modulates the circuit interactions in such a way that we don’t move too much, we don’t move too little, we don’t move too fast or too slow, and we don’t get overly repetitive in the movements that we make. We’re just right,” Graybiel says.
Parkinson’s disease develops when the neurons connecting the substantia nigra to the striatum die, cutting off a critical dopamine source; in a process that is not entirely understood, too little dopamine translates to difficulty initiating movement. Most Parkinson’s patients receive L-dopa, which can substitute for the lost dopamine. However, the effects usually wear off after five to 10 years, and complications appear.
To study exactly how dopamine loss affects the striatum, the researchers disabled dopamine-releasing cells on one side of the striatum, in rats. This mimics what usually happens in the early stages of Parkinson’s disease, when dopamine input is cut off on only one side of the brain.
As the rats learned to run a T-shaped maze, the researchers recorded electrical activity in many individual neurons. The rats were rewarded for correctly choosing to run left or right as they approached the T, depending on the cue that they heard.
The researchers focused on two types of neurons: projection neurons, which send messages from the striatum to the neocortex to initiate or halt movement, and fast-spiking interneurons, which enable local communication within the striatum. Among the projection neurons, the researchers identified two subtypes — those that were active just before the rats began running, and those that were active during the run.
In the dopamine-depleted striatum, the researchers found, to their surprise, that the projection neurons still developed relatively normal activity patterns. However, they became even more active during the time when they were usually active (before or during the run). These hyper-drive effects were related to whether the rats had learned the maze task or not.
The interneurons, however, never developed the firing patterns seen in normal interneurons during learning, even after the rats had learned to run the maze. The local circuits were disabled.
Restoring neuron function
When the researchers then treated the rats with L-dopa, the drug restored normal activity in the projection neurons, but did not bring back normal activity in the interneurons. A possible reason for that is that those cells become disconnected by the loss of dopamine, so even when L-dopa is given, they can no longer shape the local circuits to respond to it.
This is the first study to show that the effects of dopamine loss depend not only on the type of neuron, but also on the phase of task behavior and how well the task has been learned, according to the researchers. To glean even more detail, Graybiel’s lab is now working on measuring dopamine levels in different parts of the brain as the dopamine-depleted rats learn new behaviors.
The lab is also seeking ways to restore function to the striatal interneurons that don’t respond to L-dopa treatment. The findings underscore the need for therapies that target specific deficiencies, says Joshua Goldberg, a senior lecturer in medical neurobiology at the Hebrew University of Jerusalem.
The new study “refines our appreciation of the complexity of [Parkinson’s],” says Goldberg, who was not part of the research team. “Graybiel’s team drives home the message that dopamine depletion, and dopamine replacement therapy, do not affect brain dynamics or behavior in a uniform fashion. Instead, their effect is highly context-dependent and differentially affects various populations of neurons.”
The research was funded by the National Institutes of Health/National Institute of Neurological Disorders and Stroke, the National Parkinson Foundation, the Stanley H. and Sheila G. Sydney Fund, a Parkinson’s Disease Foundation Fellowship and a Fulbright Fellowship.
“We know the neurotransmitter, we know roughly the pathways in the brain that are being affected, but when you come right down to it and ask what exactly is the sequence of events that occurs in the brain, that gets a little tougher,” says Ann Graybiel, an MIT Institute Professor and member of MIT’s McGovern Institute for Brain Research.
A new study from Graybiel’s lab offers insight into some of the precise impairments caused by the loss of dopamine in brain cells affected by Parkinson’s disease. The findings, which appear in the March 12 online edition of the Journal of Neuroscience, could help researchers not only better understand the disease, but also develop more targeted treatments.
Lead author of the paper is Ledia Hernandez, a former MIT postdoc. Other authors are McGovern Institute research scientists Yasuo Kubota and Dan Hu, former MIT graduate student Mark Howe and graduate student Nuné Lemaire.
Cutting off dopamine
The neurons responsible for coordinating movement are located in a part of the brain called the striatum, which receives information from two major sources — the neocortex and a tiny region known as the substantia nigra. The cortex relays sensory information as well as plans for future action, while the substantia nigra sends dopamine that helps to coordinate all of the cortical input.
“This dopamine somehow modulates the circuit interactions in such a way that we don’t move too much, we don’t move too little, we don’t move too fast or too slow, and we don’t get overly repetitive in the movements that we make. We’re just right,” Graybiel says.
Parkinson’s disease develops when the neurons connecting the substantia nigra to the striatum die, cutting off a critical dopamine source; in a process that is not entirely understood, too little dopamine translates to difficulty initiating movement. Most Parkinson’s patients receive L-dopa, which can substitute for the lost dopamine. However, the effects usually wear off after five to 10 years, and complications appear.
To study exactly how dopamine loss affects the striatum, the researchers disabled dopamine-releasing cells on one side of the striatum, in rats. This mimics what usually happens in the early stages of Parkinson’s disease, when dopamine input is cut off on only one side of the brain.
As the rats learned to run a T-shaped maze, the researchers recorded electrical activity in many individual neurons. The rats were rewarded for correctly choosing to run left or right as they approached the T, depending on the cue that they heard.
The researchers focused on two types of neurons: projection neurons, which send messages from the striatum to the neocortex to initiate or halt movement, and fast-spiking interneurons, which enable local communication within the striatum. Among the projection neurons, the researchers identified two subtypes — those that were active just before the rats began running, and those that were active during the run.
In the dopamine-depleted striatum, the researchers found, to their surprise, that the projection neurons still developed relatively normal activity patterns. However, they became even more active during the time when they were usually active (before or during the run). These hyper-drive effects were related to whether the rats had learned the maze task or not.
The interneurons, however, never developed the firing patterns seen in normal interneurons during learning, even after the rats had learned to run the maze. The local circuits were disabled.
Restoring neuron function
When the researchers then treated the rats with L-dopa, the drug restored normal activity in the projection neurons, but did not bring back normal activity in the interneurons. A possible reason for that is that those cells become disconnected by the loss of dopamine, so even when L-dopa is given, they can no longer shape the local circuits to respond to it.
This is the first study to show that the effects of dopamine loss depend not only on the type of neuron, but also on the phase of task behavior and how well the task has been learned, according to the researchers. To glean even more detail, Graybiel’s lab is now working on measuring dopamine levels in different parts of the brain as the dopamine-depleted rats learn new behaviors.
The lab is also seeking ways to restore function to the striatal interneurons that don’t respond to L-dopa treatment. The findings underscore the need for therapies that target specific deficiencies, says Joshua Goldberg, a senior lecturer in medical neurobiology at the Hebrew University of Jerusalem.
The new study “refines our appreciation of the complexity of [Parkinson’s],” says Goldberg, who was not part of the research team. “Graybiel’s team drives home the message that dopamine depletion, and dopamine replacement therapy, do not affect brain dynamics or behavior in a uniform fashion. Instead, their effect is highly context-dependent and differentially affects various populations of neurons.”
The research was funded by the National Institutes of Health/National Institute of Neurological Disorders and Stroke, the National Parkinson Foundation, the Stanley H. and Sheila G. Sydney Fund, a Parkinson’s Disease Foundation Fellowship and a Fulbright Fellowship.