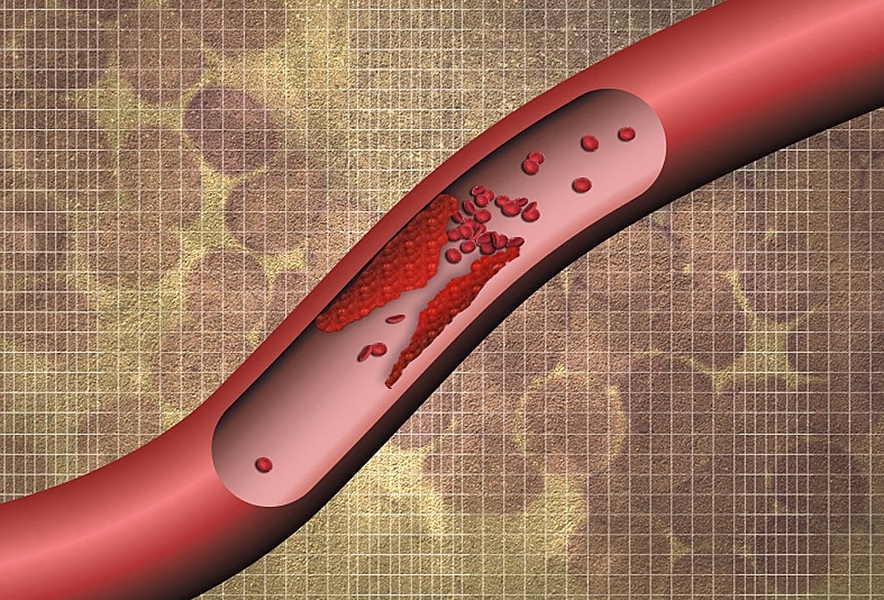
Life-threatening blood clots can form in anyone who sits on a plane for a long time, is confined to bed while recovering from surgery, or takes certain medications.
There is no fast and easy way to diagnose these clots, which often remain undetected until they break free and cause a stroke or heart attack. However, new technology from MIT may soon change that: A team of engineers has developed a way to detect blood clots using a simple urine test.
The noninvasive diagnostic, described in a recent issue of the journal ACS Nano, relies on nanoparticles that detect the presence of thrombin, a key blood-clotting factor.
Such a system could be used to monitor patients who are at high risk for blood clots, says Sangeeta Bhatia, senior author of the paper and the John and Dorothy Wilson Professor of Health Sciences and Technology and Electrical Engineering and Computer Science.
“Some patients are at more risk for clotting, but existing blood tests are not consistently able to detect the formation of new clots,” says Bhatia, who is also a senior associate member of the Broad Institute and a member of MIT’s Koch Institute for Integrative Cancer Research and Institute for Medical Engineering and Science (IMES).
Lead authors of the paper are Kevin Lin, a graduate student in chemical engineering, and Gabriel Kwong, a postdoc in IMES. Other authors are Andrew Warren, a graduate student in Health Sciences and Technology (HST), and former HST postdoc David Wood.
Sensing thrombin
Blood clotting is produced by a complex cascade of protein interactions, culminating in the formation of fibrin, a fibrous protein that seals wounds. The last step of this process — the conversion of fibrinogen to fibrin — is controlled by an enzyme called thrombin.
Current tests for blood clotting are very indirect, Bhatia says. One, known as the D-dimer test, looks for the presence of fibrin byproducts, which indicates that a clot is being broken down, but will not detect its initial formation.
Bhatia and her colleagues developed their new test based on a technology they first reported last year for early detection of colorectal cancer. “We realized the same exact technology would work for blood clots,” she says. “So we took the test we had developed before, which is an injectable nanoparticle, and made it a thrombin sensor.”
The system consists of iron oxide nanoparticles, which the Food and Drug Administration has approved for human use, coated with peptides (short proteins) that are specialized to interact with thrombin. After being injected into mice, the nanoparticles travel throughout the body. When the particles encounter thrombin, the thrombin cleaves the peptides at a specific location, releasing fragments that are then excreted in the animals’ urine.
Once the urine is collected, the protein fragments can be identified by treating the sample with antibodies specific to peptide tags included in the fragments. The researchers showed that the amount of these tags found in the urine is directly proportional to the level of blood clotting in the mice’s lungs.
In the previous version of the system, reported last December in Nature Biotechnology, the researchers used mass spectrometry to distinguish the fragments by their mass. However, testing samples with antibodies is much simpler and cheaper, the researchers say.
Rapid screening
Bhatia says she envisions two possible applications for this kind of test. One is to screen patients who come to the emergency room complaining of symptoms that might indicate a blood clot, allowing doctors to rapidly triage such patients and determine if more tests are needed.
“Right now they just don’t know how to efficiently define who to do the more extensive workup on. It’s one of those things that you can’t afford to miss, so patients can get an unnecessarily expensive workup,” Bhatia says.
Another application is monitoring patients who are at high risk for a clot — for example, people who have to spend a lot of time in bed recovering from surgery. Bhatia is working on a urine dipstick test, similar to a pregnancy test, that doctors could give patients when they go home after surgery.
“If a patient is at risk for thrombosis, you could send them home with a 10-pack of these sticks and say, ‘Pee on this every other day and call me if it turns blue,’” she says.
The technology could also be useful for predicting recurrence of clots, says Henri Spronk, an assistant professor of biochemistry at Maastricht University in the Netherlands.
“High levels of activation markers have been related to recurrent thrombosis, but they don’t have good sensitivity or specificity. Through application of the nanoparticles, if proven well-tolerated and nontoxic, alterations in the normal low levels of physiological thrombin generation might be easily detected,” says Spronk, who was not part of the research team.
Bhatia plans to launch a company to commercialize the technology, with funding from MIT’s Deshpande Center for Technological Innovation. Other applications for the nanoparticle system could include monitoring and diagnosing cancer. It could also be adapted to track liver, pulmonary, and kidney fibrosis, Bhatia says.
The research was funded by the Koch Institute Frontier Research Fund, the Kathy and Curt Marble Cancer Research Fund, the Mazumdar-Shaw International Oncology Fellows Program, the Burroughs Wellcome Fund, and the Deshpande Center.
There is no fast and easy way to diagnose these clots, which often remain undetected until they break free and cause a stroke or heart attack. However, new technology from MIT may soon change that: A team of engineers has developed a way to detect blood clots using a simple urine test.
The noninvasive diagnostic, described in a recent issue of the journal ACS Nano, relies on nanoparticles that detect the presence of thrombin, a key blood-clotting factor.
Such a system could be used to monitor patients who are at high risk for blood clots, says Sangeeta Bhatia, senior author of the paper and the John and Dorothy Wilson Professor of Health Sciences and Technology and Electrical Engineering and Computer Science.
“Some patients are at more risk for clotting, but existing blood tests are not consistently able to detect the formation of new clots,” says Bhatia, who is also a senior associate member of the Broad Institute and a member of MIT’s Koch Institute for Integrative Cancer Research and Institute for Medical Engineering and Science (IMES).
Lead authors of the paper are Kevin Lin, a graduate student in chemical engineering, and Gabriel Kwong, a postdoc in IMES. Other authors are Andrew Warren, a graduate student in Health Sciences and Technology (HST), and former HST postdoc David Wood.
Sensing thrombin
Blood clotting is produced by a complex cascade of protein interactions, culminating in the formation of fibrin, a fibrous protein that seals wounds. The last step of this process — the conversion of fibrinogen to fibrin — is controlled by an enzyme called thrombin.
Current tests for blood clotting are very indirect, Bhatia says. One, known as the D-dimer test, looks for the presence of fibrin byproducts, which indicates that a clot is being broken down, but will not detect its initial formation.
Bhatia and her colleagues developed their new test based on a technology they first reported last year for early detection of colorectal cancer. “We realized the same exact technology would work for blood clots,” she says. “So we took the test we had developed before, which is an injectable nanoparticle, and made it a thrombin sensor.”
The system consists of iron oxide nanoparticles, which the Food and Drug Administration has approved for human use, coated with peptides (short proteins) that are specialized to interact with thrombin. After being injected into mice, the nanoparticles travel throughout the body. When the particles encounter thrombin, the thrombin cleaves the peptides at a specific location, releasing fragments that are then excreted in the animals’ urine.
Once the urine is collected, the protein fragments can be identified by treating the sample with antibodies specific to peptide tags included in the fragments. The researchers showed that the amount of these tags found in the urine is directly proportional to the level of blood clotting in the mice’s lungs.
In the previous version of the system, reported last December in Nature Biotechnology, the researchers used mass spectrometry to distinguish the fragments by their mass. However, testing samples with antibodies is much simpler and cheaper, the researchers say.
Rapid screening
Bhatia says she envisions two possible applications for this kind of test. One is to screen patients who come to the emergency room complaining of symptoms that might indicate a blood clot, allowing doctors to rapidly triage such patients and determine if more tests are needed.
“Right now they just don’t know how to efficiently define who to do the more extensive workup on. It’s one of those things that you can’t afford to miss, so patients can get an unnecessarily expensive workup,” Bhatia says.
Another application is monitoring patients who are at high risk for a clot — for example, people who have to spend a lot of time in bed recovering from surgery. Bhatia is working on a urine dipstick test, similar to a pregnancy test, that doctors could give patients when they go home after surgery.
“If a patient is at risk for thrombosis, you could send them home with a 10-pack of these sticks and say, ‘Pee on this every other day and call me if it turns blue,’” she says.
The technology could also be useful for predicting recurrence of clots, says Henri Spronk, an assistant professor of biochemistry at Maastricht University in the Netherlands.
“High levels of activation markers have been related to recurrent thrombosis, but they don’t have good sensitivity or specificity. Through application of the nanoparticles, if proven well-tolerated and nontoxic, alterations in the normal low levels of physiological thrombin generation might be easily detected,” says Spronk, who was not part of the research team.
Bhatia plans to launch a company to commercialize the technology, with funding from MIT’s Deshpande Center for Technological Innovation. Other applications for the nanoparticle system could include monitoring and diagnosing cancer. It could also be adapted to track liver, pulmonary, and kidney fibrosis, Bhatia says.
The research was funded by the Koch Institute Frontier Research Fund, the Kathy and Curt Marble Cancer Research Fund, the Mazumdar-Shaw International Oncology Fellows Program, the Burroughs Wellcome Fund, and the Deshpande Center.